A 69-Year-Old Man Who Quietly Changed His Numbers
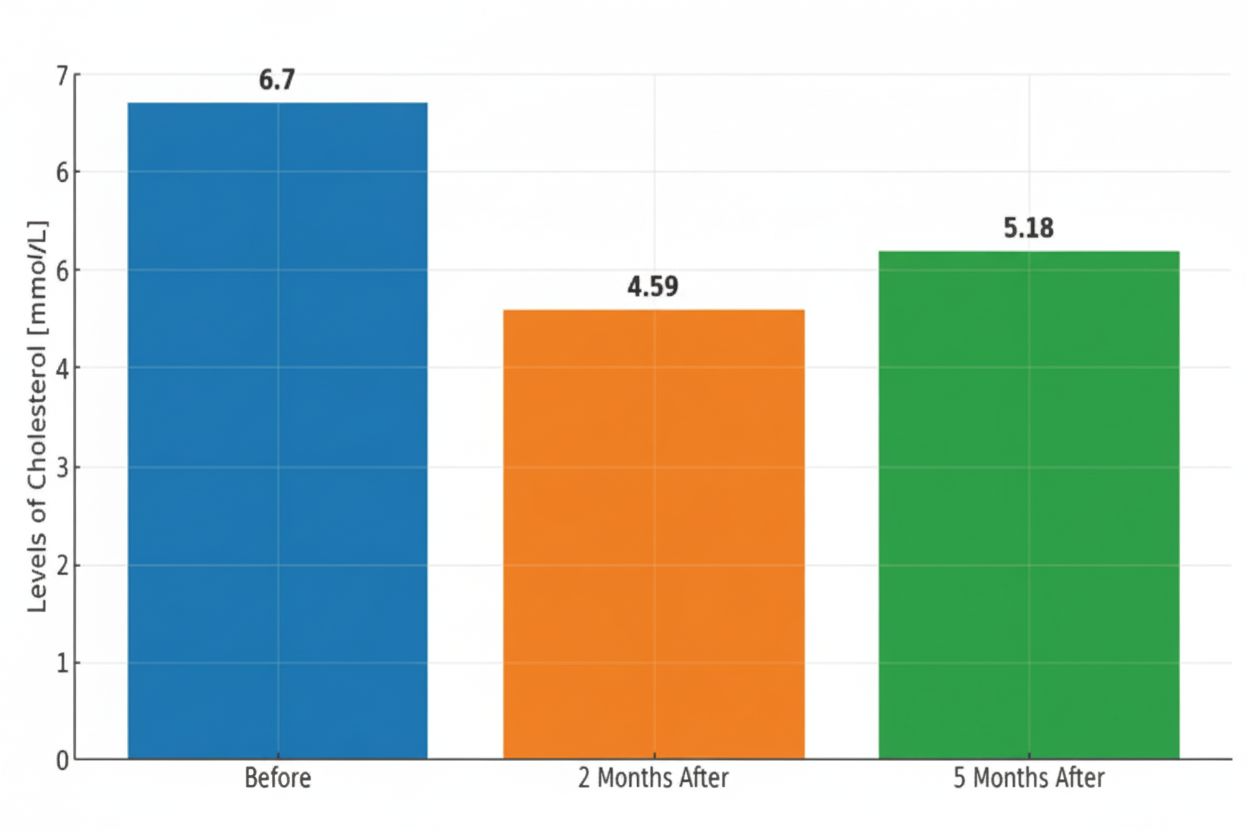
Fig. 1 — Documented changes in the patient's lipid panel over the observation period
What's remarkable about this case is not just that his levels improved — it's why they did. To understand this, we need to revisit the basics of how cholesterol actually works in the body. Because most of what people believe about it is, quite simply, wrong.
The Problem Isn't What You Eat.
It Never Was.
produced by your liver
you eat each day
Your liver is the master regulator of cholesterol. It synthesizes it, recycles it, and — critically — removes excess cholesterol from your bloodstream. When your levels run high, the question isn't "how do I stop eating cholesterol?" The real question is: why is the liver failing to regulate it properly?
Cutting saturated fat or switching to a "heart-healthy" diet may nudge your numbers by a few percent. But if your liver's regulatory function is impaired, those changes barely register. You're managing a symptom while the underlying cause continues unchecked.
When cholesterol is elevated, the liver already knows about it. It has dedicated sensors designed to detect and correct exactly this. If it isn't correcting it, something is preventing the liver from doing its job — and that something needs to be addressed directly, not masked.
When Cholesterol Is Elevated, the Liver Is Working at Its Limit —
But Still Can't Cope. Why?
The Liver Needs Energy to Regulate Cholesterol — And That Energy Has a Source
The liver is one of the most energy-intensive organs in the human body. Every biochemical process it carries out — including cholesterol regulation — requires a constant supply of cellular energy.
That energy is produced by mitochondria. You may remember them from school biology — they're often called "the powerhouses of the cell." Each liver cell contains thousands of them. When mitochondrial function deteriorates, the liver simply doesn't have enough energy to perform its work properly and regulate cholesterol effectively.
This is exactly why cholesterol problems so often appear — or get significantly worse — after the age of 45–55. That's precisely when mitochondrial efficiency naturally begins to decline in most people. It isn't a question of willpower or diet. It's cellular biology.
Why Statins and Diet
Don't Produce the Results You Need
If you've been told to watch your diet or take statins, you're not alone. These are the two most common recommendations for high cholesterol — and both miss the point entirely.
68 Patients Normalized Mitochondrial Function and
Restored Healthy Cholesterol Levels — Without Diet or Exercise
The link between hepatic energy metabolism and cholesterol levels has already been studied and officially documented at one of the world's most respected scientific research institutions. The connection is no longer theoretical — it has been measured, recorded, and published.
A landmark study was conducted examining the relationship between cellular energy metabolism and lipid regulation in patients with metabolic syndrome
68 participants with metabolic syndrome were enrolled — all presenting with elevated cholesterol, impaired glucose regulation, and markers of hepatic stress. Participants were monitored over a structured observation period. Researchers measured changes in lipid panels, metabolic markers, and liver function indicators. Importantly, participants did not follow special diets and did not begin exercise programs. The study's sole focus was on supporting mitochondrial function using a single compound.
The results across all 68 participants were consistent. These weren't people who radically overhauled their lifestyles. The intervention worked at a cellular level — by restoring the liver's energy deficit, the liver was finally able to do what it was always designed to do. No suppression. No workarounds. Just the liver functioning as it should.
Mitochondrial dysfunction in hepatocytes is increasingly recognized as a central mechanism in the development of dyslipidemia. Restoring mitochondrial activity represents a fundamentally different — and more targeted — therapeutic approach than conventional lipid-lowering strategies.
Two entirely separate groups of people. Different ages, different health profiles, different circumstances. Yet in both cases, their cholesterol markers moved in the right direction — without drastic dietary changes. The one question worth asking: what did they all have access to?


Both Studies Involved the Same Mineral: Synthesit
Synthesit is a unique bioavailable mineral compound developed to support cellular energy metabolism. Its mechanism centers on mitochondrial function — specifically, the mitochondria in liver cells responsible for powering the body's natural cholesterol regulation.
Unlike statins, which suppress cholesterol synthesis entirely and carry a well-documented list of side effects, Synthesit works with your body's own systems. It gives the liver the cellular resources it needs to regulate cholesterol naturally — the way it was designed to before mitochondrial decline set in.
This is why the results across both the published case report and the 68-participant clinical study showed consistent, measurable improvements in lipid profiles — without extreme lifestyle interventions. The liver was simply given back its energy.
Find out more about the mineral behind both studies
What Is Synthesit? →Learn about the research, the mechanism, and how to get it

